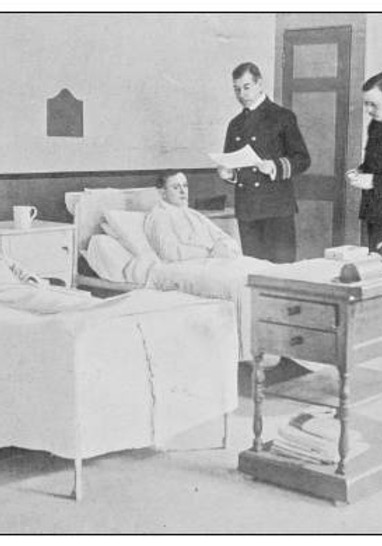
DOCTOR

INFORMATION
Perhaps no career was so well-regarded in any century as that of the doctor. From practitioners of modern westernized medicine, to more traditional eastern remedies - cures for ailments both physical and spiritual made by voodoo practitioners or even the medicine men of some indigenous tribes, no society could survive without someone to tend wounds and keep illness at bay.
Doctors come in a vast array of exact flavors. From physicians and surgeons, midwives and nurses, or even healers who belong to cultures outside of the westernized norm, anyone who wishes to deal in medicine can fall under this career type.
REQUIREMENTS
Doctors are considered equal-opportunity. Characters of any race, gender, or presentation will have an equal review in these applications.
BENFITS
-
Base Paycheck of $20.00
-
Access to Doctor's Craftbook
-
Access to Medical License
GUIDELINES
Doctors may utilize the role to portray themselves as physicians, surgeons, midwives, nurses, folk-healers, or any other path related to the treatment of illnesses and injuries through medicine. Doctors are encouraged but not required to work at clinic properties.
A certain degree of realism and proper portrayal is expected in the roleplay of a doctor - a detailed guide of integrating realism into your roleplay is listed below. Additionally, the portrayal of folk medicine and healing will be highly scrutinized for respectful portrayal.
ROLEPLAYING A DOCTOR
A doctor in the United States in the late 1800s was a professional straddling the line between traditional practices and the emerging world of modern medicine. Physicians were respected, but medicine was not yet the prestigious, high-tech field it would become. In rural areas, the local doctor might also serve as a dentist, pharmacist, and even a coroner. Their work was grueling, and they were often on call at all hours, traveling long distances to see patients. Doctors could often be found in a small-town clinic, a city hospital, or making house calls across rural roads. Doctor’s offices would typically have smelled of alcohol and antiseptics, or sometimes laudanum. Their office furnishings were simple: a wooden desk, shelves lined with glass bottles, and a well-worn examination table. They were typically dedicated generalists, working in a time of transition, using old remedies with new science, serving their community with limited tools but growing knowledge. Doctors in this time usually operated solo practitioners or with one assistant and had to rely on their own judgment, tools, and courage.
Treatments typically relied on rudimentary procedures. Bloodletting had mostly fallen out of favor, but purgatives, tonics, and opiates like laudanum were still common. Germ theory was gaining ground, especially after Joseph Lister's promotion of antiseptic surgery in 1867. Anesthesia such as ether and chloroform were in use, though risky. X-rays wouldn’t be discovered until 1895, and antibiotics were decades away. Doctors also played roles in sanitation and public health, especially as urban populations grew. They dealt with outbreaks of diseases like typhoid, tuberculosis, and diphtheria, often with limited means.
Because of the absence of advanced medical equipment, the tools used were typically basic, such as bone saws, knives, and leather straps. Headaches were sometimes attempted to be relieved with trepanning, the act of drilling a hole in the skull to relieve the pressure. Surgeries were often performed without anesthesia, typically with only chloroform or whiskey. Limbs were sometimes amputated to prevent infection, even if survival wasn’t guaranteed. These technique were administered due to a lack of technology and equipment that was typically only available in hospitals.
Due to most doctors being self-taught sometimes more unconventional remedies were used such as whiskey, herbs, poultices, leeches, opium, home-brewed tonics, and even turpentine. Some might have even leaned on spirituality, astrology, or “bad humors” to explain illnesses. Some believed in balancing the four humors (blood, phlegm, black bile, yellow bile) which came from an ancient medieval medical system called humorism.
Doctors in this time had to be very versatile usually treating a little bit of everything like gunshot wounds, childbirth, amputations, fevers, dental work, and even mental illness. They were often the only medical help for miles, with no hospitals in close range. Actual hospitals were usually only located in major cities, requiring doctors in rural areas to be the go to source for all ailments.
Most doctors in the late 1800s were self-taught or only had brief inconsistent training. Some were trained by other doctors through short apprenticeships. Medical schools existed but varied in quality and most only offered 2 years of lecture-based education and lacked hands-on training. Licensing was just beginning to be standardized and only a few doctors had hospital residences.
Due to these harsh conditions many doctors became hardened or numb to illness and disease after dealing with death, pain, and panic as a daily occurrence. It was a very taxing and exhausting position and took a dedicated individual to fill the role.
Within the community doctors were often seen as saviors but most times were only utilized as a last resort. Townsfolk would often only seek help from a doctor after exhausting other sources like superstition, prayer, or herbal cures first.
In the State of Lavinia doctors will treat all sorts of wounds and illnesses, ranging from gunshot wounds to cholera to hysteria. Once you have received the role as a doctor, you have the choice to apply to own one of our various doctor clinics, work as an apprentice to a leading doctor, or simply become a traveling doctor roaming the state helping patients.
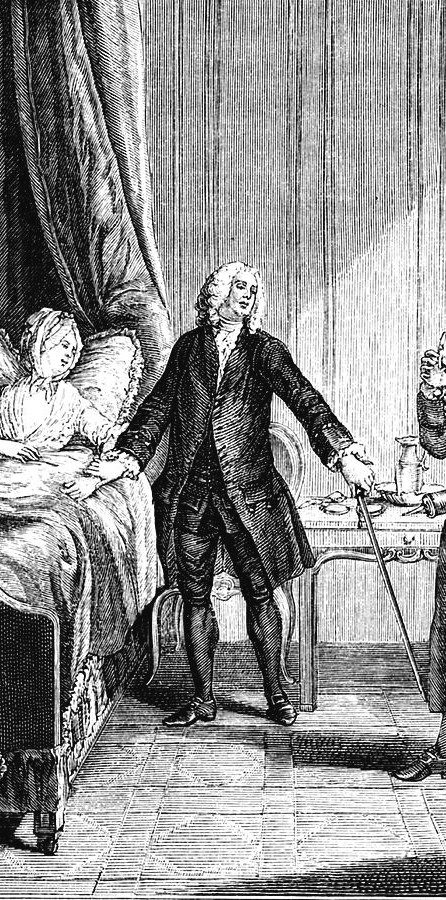

DUTIES & RESPONSIBILITIES
In the late 1800s, the duties and responsibilities of doctors were significantly different from today’s standards due to limited medical knowledge, rudimentary technology, and less formalized professional structures. However, their core mission remained the same: to care for the sick and injured.
Diagnosing and Treating Illnesses
-
Doctors used limited diagnostic tools, relying heavily on observation, patient descriptions, and basic instruments like stethoscopes and thermometers.
-
Common treatments included the use of tonics or herbal remedies.
-
Diseases like tuberculosis, typhoid, and cholera were common, and treatments were often ineffective by modern standards.
-
Mortality rates were often elevated during outbreaks of infectious diseases due to lack of proper medication and the inability to consult with other medical professionals.
Performing Minor Surgeries
-
Some doctors performed minor surgical procedures, especially in rural areas, without access to trained surgeons.
-
Surgery was risky due to lack of anesthesia and there was a poor understanding of infection control until antiseptic practices were introduced by Lister in 1867.
House Calls
-
Most doctors made house visits, as hospitals were few and often avoided due to poor conditions.
-
They traveled by horseback or carriage, sometimes covering long distances, especially in rural areas.
Childbirth Assistance
-
General practitioners often acted as midwives, especially in rural or underserved areas.
-
They typically delivered babies in patients’ homes and managed complications as best they could.
Public Health and Disease Prevention
-
Doctors sometimes advised on sanitation, quarantine practices, and public health measures, especially during outbreaks.
-
The late 1800s saw growing awareness of germ theory, especially after Pasteur and Koch’s discoveries.
Record Keeping
-
Doctors maintained basic patient records, usually handwritten in notebooks.
-
These records included symptoms, treatments given, and progress of current patients.
Dispensing Medicines
-
Many doctors compounded and dispensed their own medicines, as pharmacies were not always accessible.
-
They used patent medicines, some of which contained alcohol, opium, or other now-controlled substances.
Education and Self-Improvement
-
Doctors were expected to stay informed about new medical developments, though access to journals and formal continuing education was limited.
-
Some participated in medical societies or attended lectures, when possible, but many had limited medical knowledge other than self-taught experience.
Ethical and Social Responsibilities
-
Doctors were held in high regard in their communities and were expected to uphold moral and professional behavior.
-
Confidentiality, though not formalized like today, was generally respected.
-
They often provided care regardless of ability to pay, especially in small communities.


ETHICS & MORALS
The ethics and morals of doctors in the late 1800s were shaped by a mix of evolving scientific understanding, professional codes, societal expectations, and deeply rooted traditions. While there was no universal ethical code comparable to modern standards, there were important developments and attitudes that influenced medical practice during this time.
Doctors in the late 1800s were in a transitional period, moving from a more informal, gentleman-practitioner model to a professional, science-based one. Ethics were professionally guided but not strictly regulated. Their ethics were heavily influenced by social values, which were often biased and paternalistic. Their practices were still lacking in many protections we now consider standard, like informed consent or non-discriminatory care.
In 1847, the American Medical Association (AMA) adopted one of the first formal codes of medical ethics, inspired by Thomas Percival’s Medical Ethics written in 1803 in England. These codes stressed the importance of responsibilities towards patients, including honesty, beneficence, and confidentiality. They also outlined professional conduct for doctors, such as avoiding quackery, respecting peers, and moral character meaning doctors were expected to be virtuous and self-regulating.
Physicians often practiced paternalistic care, meaning they made decisions for patients without necessarily informing them fully or seeking consent. The idea was that the doctor “knew best,” and patients were seen as incapable of fully understanding medical complexities. The concept of informed consent did not formally exist. Doctors often withheld information from patients if they believed it was in the patient’s best interest. Ethical scrutiny of this practice would only emerge in the 20th century.
The late 1800s also saw an increase in scientific research, but the ethics of human experimentation were loose or nonexistent. Some doctors conducted clinical trials or surgeries without patient knowledge or approval. There were few consequences for ethical breaches, especially when experiments involved marginalized groups.
Ethics were frequently shaped by social hierarchies:
-
Poor patients, women, and racial minorities often received substandard care or were used as subjects for experimentation without consent. For example, Black patients in the U.S. South were often exploited in teaching hospitals or used in unethical research.
-
Women’s health was often misunderstood or dismissed (e.g., diagnoses like “hysteria”).
Morals also varied from doctor to doctor. Some truly cared for their patients and thought they were administering the best possible treatment, others had become hardened after witnessing so much trauma and lost their desire to feel empathy, and others had more sinister motives for their profession such as using patients as guinea pigs to further experimentation or simply because they enjoyed in the act of witnessing and inflicting pain.
In Lavinia, we welcome all types of doctoral roles, we’ll leave it up to your interpretation on how you wish to proceed forward in the care or lack of care when treating citizens of the state.
WOMEN IN MEDICINE
In the late 1800s, the role of female doctors was groundbreaking, highly limited, and often controversial. Women who pursued careers in medicine during this time encountered major social, institutional, and professional obstacles. However, some were able to overcome gender stigma, carve out meaningful roles, and make lasting contributions to both healthcare and women's rights.
Female doctors were very rare in the late 1800s, but not unheard of. Most women in medicine were pressured into becoming nurses or midwives to fit the mold of the ideology at the time. Medical schools often refused female applicants; those that did accept them were considered controversial. Many people (including male doctors) believed that women were emotionally or intellectually unfit for medicine. Female doctors were often restricted to treating women and children, which allowed them to practice but also reinforced gendered limitations. Many were relegated to serving populations that male physicians often overlooked or ignored.
A few women's medical colleges were then founded like the Woman’s Medical College of Pennsylvania which was established in 1850. But the majority of medical schools still only accepted male students up until the late 1800s. Licensing and legal recognition was difficult but was improving in parts of the U.S.
Even though women’s medical schools were emerging, women were still often banned from medical societies, hospitals, and academic posts. Female doctors were accused of being “unnatural” or “unfeminine” and many were socially isolated or harassed.
Thanks to the courageous efforts of female doctors who challenged stereotypes and demonstrated that women could excel in science and medicine, more opportunities for women in the medical field began to emerge by the late 1800s. Their work not only expanded access to medical education but also sparked reforms for gender equality in medicine. Despite facing numerous obstacles, their contributions played a crucial role in laying the groundwork for greater gender inclusion in the medical profession.